Published: 21 March 2026 | Medically reviewed | Last updated: 21 March 2026
What to Avoid With Diabetic Retinopathy?
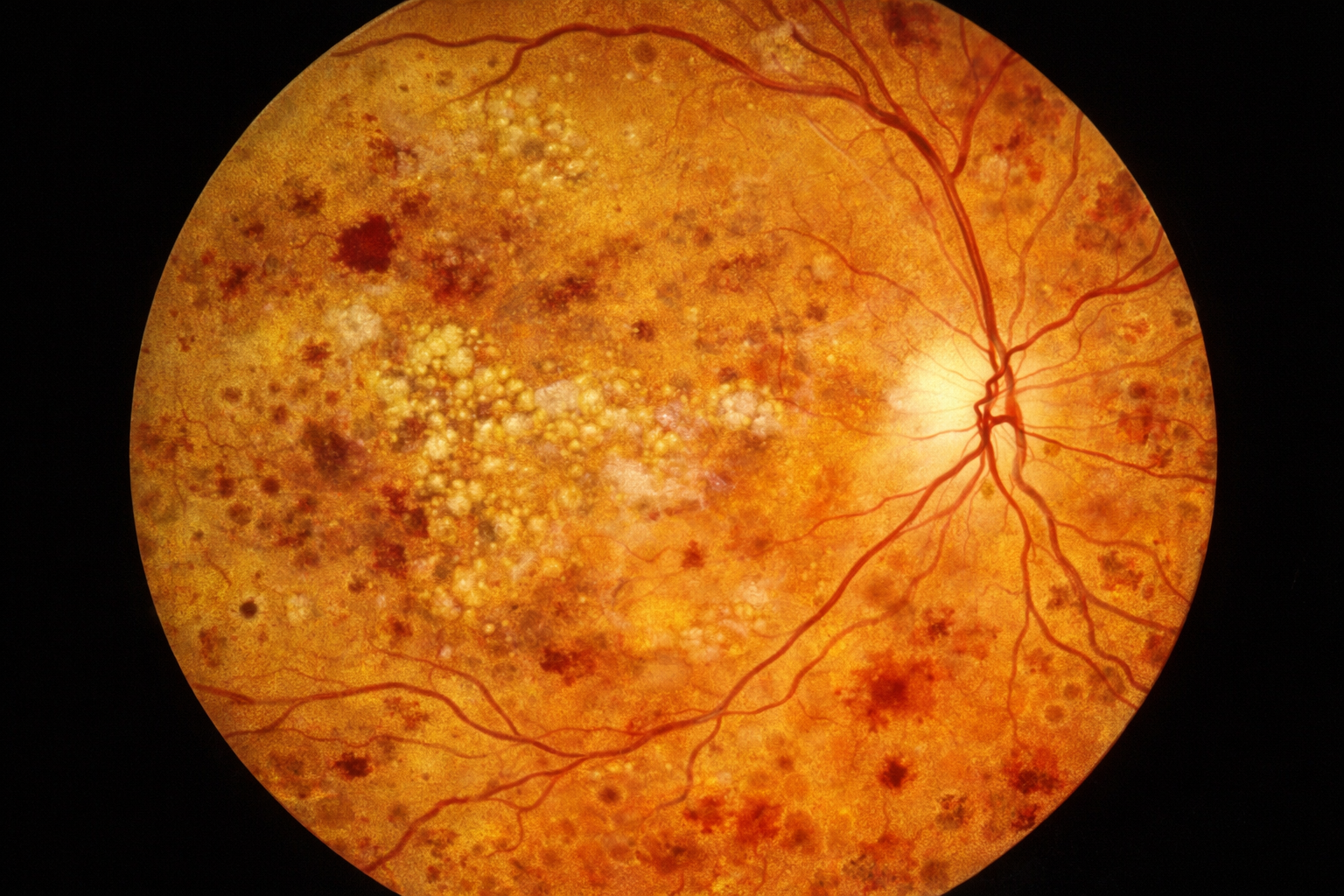
Diabetic retinopathy is an eye disease caused by damage to the small blood vessels in the retina from diabetes. It can begin silently, without obvious symptoms, and then gradually lead to blurred vision, floaters, dark areas in vision, diabetic macular edema, bleeding inside the eye, retinal detachment, and permanent sight loss if it progresses. Because of that, the question is not only how to treat diabetic retinopathy, but also what to avoid so it does not worsen faster.
The most important thing to understand is this: there is no single food, supplement, or eye drop that causes or prevents diabetic retinopathy on its own. What usually makes diabetic retinopathy worse is a pattern of poor diabetes control, missed eye care, delayed treatment, and uncontrolled risk factors such as high blood pressure, high cholesterol, and smoking.
Quick summary: If you have diabetic retinopathy, avoid poor blood sugar control, uncontrolled blood pressure and cholesterol, smoking, skipping eye screening, ignoring vision changes, delaying treatment, and self-managing with home remedies instead of medical care. If you have severe or proliferative diabetic retinopathy, ask your eye specialist before doing heavy lifting, high-impact exercise, or activities that involve straining.
1. Avoid Letting Blood Sugar Stay High
Persistently high blood glucose is one of the main drivers of diabetic retinopathy progression. Over time, high sugar levels damage the tiny blood vessels that nourish the retina. These vessels may weaken, leak, close off, or trigger the growth of fragile abnormal new vessels. The longer blood glucose stays poorly controlled, the greater the risk of worsening retinopathy and vision loss.
That means one of the biggest things to avoid is assuming that eye disease can be managed separately from diabetes. Good eye care starts with good diabetes control. For many people, that includes taking diabetes medication as prescribed, monitoring glucose appropriately, following a realistic meal plan, and staying physically active within safe limits.
2. Avoid Uncontrolled Blood Pressure and Cholesterol
Diabetic retinopathy is not only about blood sugar. High blood pressure and high cholesterol also increase the risk of retinal damage and can accelerate progression. Blood pressure that remains high puts additional stress on already vulnerable retinal vessels, while abnormal lipids are linked to worsening retinal leakage and complications.
So if you have diabetic retinopathy, avoid neglecting your blood pressure and cholesterol targets. Eye disease often reflects the health of your blood vessels more broadly, not just your glucose level.
3. Avoid Smoking
Smoking is another major habit to avoid. Smoking increases vascular stress, worsens overall diabetes risk, and is associated with a higher risk of diabetes-related eye disease. It also harms cardiovascular health, which matters because diabetic retinopathy is fundamentally a disease of damaged circulation in the retina.
If you smoke and have diabetic retinopathy, quitting is one of the most important steps you can take for both your eyes and your general health.
4. Avoid Skipping Dilated Eye Exams Because Your Vision “Seems Fine”
One of the most dangerous mistakes is skipping diabetic eye screening or full dilated eye exams because you think your sight is normal. Early diabetic retinopathy often causes no symptoms at all. Damage may already be developing long before you notice blurred vision or floaters.
That is why regular eye examinations are so important. They allow retinal changes to be detected early, often before major vision loss occurs. Missing those visits can delay diagnosis until the disease is much harder to control.
5. Avoid Ignoring New Vision Changes
Do not ignore changes such as:
- Blurred vision
- Floaters or dark spots
- Flashes of light
- Dark or empty areas in vision
- Distortion of straight lines
- Trouble reading or doing detail work
- Sudden loss of vision
Some people assume these symptoms will settle on their own. That can be risky. In diabetic retinopathy, new symptoms may mean bleeding into the vitreous, swelling in the macula, traction on the retina, or retinal detachment. The earlier these problems are assessed, the better the chance of protecting sight.
Seek urgent eye care immediately if you have diabetic retinopathy and suddenly develop severe blurred vision, a shower of floaters, flashes, a curtain or shadow across your vision, or any sudden drop in sight. These may be warning signs of bleeding, retinal traction, or retinal detachment.
6. Avoid Delaying Recommended Treatment
If your eye specialist recommends treatment, avoiding or postponing it without medical advice can lead to preventable vision loss. Depending on the stage of disease, treatment may include:
- Anti-VEGF eye injections
- Laser treatment
- Steroid treatment in selected cases
- Vitrectomy surgery for severe bleeding or traction
Many people feel anxious about injections or laser treatment and may be tempted to wait. But diabetic retinopathy often responds best when treated before major irreversible vision loss has happened. Delaying care can allow swelling, bleeding, scarring, and traction to worsen.
7. Avoid Stopping Diabetes or Blood Pressure Medicines on Your Own
Another important thing to avoid is changing or stopping medicines without guidance from your diabetes team. Because diabetic retinopathy is closely tied to blood sugar, blood pressure, and cholesterol control, stopping medication can quickly increase the risk of worsening retinal damage.
If you are having side effects, cost concerns, or trouble sticking with treatment, the safer approach is to speak with your clinician and adjust the plan properly rather than abandoning treatment.
8. Avoid Relying on Supplements or Home Remedies Instead of Proper Care
There is no evidence that vitamins, herbs, juices, or internet remedies can replace proper diabetic retinopathy treatment. Some people delay essential care because they hope diet changes alone, eye exercises, or supplements will reverse established retinal disease. While a healthy diet is important for diabetes management, it is not a substitute for eye examinations and medically appropriate treatment.
Diabetic retinopathy is a retinal vascular disease. If it has progressed to macular edema, proliferative disease, vitreous hemorrhage, or traction, medical treatment may be needed to prevent lasting visual damage.
9. Avoid Heavy Lifting, Straining, or Vigorous High-Impact Exercise if You Have Severe or Proliferative Disease Until You Have Specialist Advice
Exercise is generally good for diabetes and eye health overall, but in severe non-proliferative diabetic retinopathy, untreated proliferative diabetic retinopathy, or after some recent eye procedures, certain activities may need to be avoided temporarily. Heavy lifting, breath-holding during exertion, straining, head-down positions, jarring high-impact exercise, or very vigorous activity can increase pressure-related stress and may raise the risk of vitreous hemorrhage or retinal complications in unstable disease.
This does not mean everyone with diabetic retinopathy should avoid exercise. In many cases, moderate low-impact activity such as walking, cycling, or water-based exercise is beneficial. The key point is to avoid guessing. If your retinopathy is advanced, ask your ophthalmologist what types of activity are safe for you.
10. Avoid Missing Extra Eye Checks During Pregnancy if You Have Pre-Existing Diabetes
Pregnancy can make diabetic retinopathy worsen more quickly in people who already have type 1 or type 2 diabetes. That is why eye checks before pregnancy or early in pregnancy are especially important. If you already have diabetes and become pregnant, avoid skipping these additional retinal assessments, even if your vision seems unchanged.
This is a special situation where retinopathy can progress faster, so close monitoring matters more than usual.
11. Avoid Assuming Blurry Vision Just Means You Need New Glasses
Blood sugar changes can temporarily alter vision, and diabetic retinopathy itself can also cause blurring. So another thing to avoid is assuming any blurred vision can be fixed with an updated glasses prescription. Sometimes the real issue is retinal swelling, fluctuating glucose, or more advanced retinal damage.
If your vision has changed, especially if the change is sudden or inconsistent, it is safer to have the underlying cause assessed rather than just ordering new glasses.
Final Answer
If you have diabetic retinopathy, avoid anything that allows retinal damage to progress silently. That includes poor blood sugar control, uncontrolled blood pressure and cholesterol, smoking, missed eye exams, ignored vision symptoms, delayed treatment, and self-treatment instead of proper medical care.
And if you have advanced or proliferative diabetic retinopathy, avoid heavy lifting, straining, and vigorous high-impact exercise unless your eye specialist says it is safe. The goal is not only to treat diabetic retinopathy, but to avoid the habits and delays that make permanent vision loss more likely.
Have questions about diabetic retinopathy?
Ask an eye doctor at
WebEyeClinic
for trusted guidance on symptoms, diabetic eye screening, treatment options, and urgent warning signs.
This article is for educational purposes only and does not replace medical advice, diagnosis, or treatment. Diabetic retinopathy can be asymptomatic in the early stages, so regular dilated eye exams and prompt specialist care are important. Medically reviewed | Last updated: 21 March 2026.